How to use your Aviva cover
Follow these steps to avoid delays:
1) Get your referral (including Aviva Digital GP)
If you’ve received a referral through the Aviva Digital GP app, we accept it directly. If you have a GP referral letter instead, that’s also fine.
2) Enquire with your Aviva details
Tell us what you need (consultation, diagnostics, treatment) and share your Aviva membership/claim details if you have them.
3) Named consultant check (if your policy requires it)
Some Aviva policies require the referral to name a specific consultant. If you’re unsure, enquire and we’ll guide you on what Aviva typically needs and how to align the referral to avoid rework.
4) Pre-authorisation and booking
Once your referral and pre-authorisation are in place, we’ll book you in and confirm what’s covered, including any excess or outpatient limits that apply.
What to have ready
If possible, have the following:
- Aviva membership details (or claim reference if you have one)
- Your referral (GP or Aviva Digital GP)
- Whether your policy needs a named consultant (if you know)
- Any excess amount noted on your policy
- A brief summary of your symptoms or the service you’re seeking
Don’t worry if you don’t have everything yet – you can still enquire and we’ll tell you what’s needed next.
FAQs for Aviva patients
Yes. If you’ve been referred via Aviva’s Digital GP app, we accept the referral directly..
Yes. This is a common Aviva requirement. If you enquire, we’ll help you confirm the correct consultant pathway so the referral matches what Aviva expects and you can proceed without delays
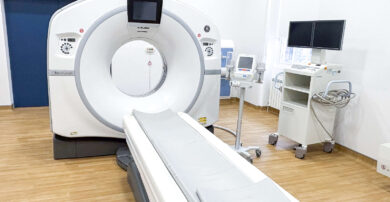
Many Aviva policies include an annual outpatient allowance. Diagnostics (such as scans) can deduct from that limit. If you’re unsure what your remaining allowance is, we recommend checking with Aviva, and we can help you understand what information Aviva typically needs for approval.
Possibly. Many policies include an excess and some items may not be covered. We’ll help you understand what applies during booking so there are no surprises.